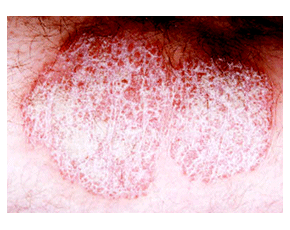
Cases of new onset psoriasis in patients receiving TNF inhibitors for the treatment of rheumatoid arthritis (RA) have been reported; however, case reports do not permit the calculation of drug-associated incidence rates. Here, Harrison et al (Ann Rheum Dis 2009; 68: 209) compare incident psoriasis in TNF inhibitor treated vs. untreated patients enrolled in the British Society for Rheumatology Biologics Register (BSRBR)
Methods
Biologic-treated RA patients enrolled in the BSRBR were compared to a comparison cohort of non-biologic treated patients for incident psoriasis. Those identified by their treating rheumatologist with new-onset psoriasis were followed up with a questionnaire querying past history of psoriasis, family history, time on TNF inhibitor to the development of psoriasis, extent of skin involvement, whether the TNF inhibitor was discontinued, and whether psoriasis improved with discontinuation. Dermatologist confirmation of psoriasis was not included.
Results
A total of 12,706 RA subjects enrolled in the BSRBR were included (n=9,826 receiving TNF inhibitor therapy, and n=2,880 from the comparison cohort). TNF inhibitor treated patients were younger, on average, than those in the comparison cohort (60 vs. 56 years, respectively; p<0.001), with higher median HAQ and DAS28 scores at enrollment. Of the TNF inhibitor treated patients, 40% received etanercept, 33% received infliximab, and 28% received adalimumab as their first TNF inhibitor. Baseline characteristics did not substantially differ by TNF inhibitor. The median follow-up time was 2.8 years for the TNF inhibitor treated patients and 1.91 years for the comparison cohort.
During follow-up, there were 42 cases of psoriasis reported, of which 36 returned follow-up questionnaires. In 25, psoriasis was new-onset in patients who were confirmed on TNF inhibitor therapy at the time of psoriasis incidence. Based on these findings, the crude rate of incident psoriasis was 1.04 per 1000 person years, compared to no cases in the non-TNF inhibitor treated group. Creating a hypothetical case in the comparison group yielded an unadjusted incidence rate ratio of 5.4 (95%CI 0.7 – 40.3) for psoriasis comparing TNF inhibitor use to non-use. Of the 25 patients with incident psoriasis, 13 (52%) received adalimumab, and 6 each (24%) for etanercept and infliximab, yielding an increased and statistically significant incidence rate ratio for adalimumab compared to no TNF inhibitor use (IRR 9.6 (95%CI 1.2-77.8). Adjusting for age, gender, smoking, and year of enrollment, the risk of psoriasis in adalimumab treated patients was also significantly higher than for treatment with etanercept and infliximab.
TNF inhibitor therapy was discontinued in 8 of the 25 patients reporting new-onset psoriasis, among whom 6 reported improvement after discontinuation. Psoriasis occurring within the first 6 months of TNF inhibitor use was reported in 13 of the 25 patients (52%), among whom 4 discontinued therapy, with 3 of these reporting improvement in psoriasis.
Conclusions
TNF inhibitor use was associated with higher rates of new-onset psoriasis in RA patients. Adalimumab was associated with a greater risk than etanercept or infliximab. Discontinuation of TNF inhibition was frequently associated with improvement in psoriasis.
Editorial Comment
Case reports have drawn attention to the potential for psoriasis in TNF inhibitor treated patients. This study expands on those by establishing rates of incident psoriasis for the first time. Overall, the risk appears to be extremely small, with mild disease fairly common, since several of the patients did not stop TNF inhibitor therapy when psoriasis appeared. The added risk associated with adalimumab is interesting, yet the immunologic basis for this difference is difficult to construct.
There is always the possibility, raised by the authors in their discussion, that the patients who developed psoriasis actually had psoriatic arthritis mimicking RA, and later developed psoriasis after the onset of arthritis. Unfortunately, this is a possibility that is exceedingly difficult to prove. However, if this was the case, one would not have expected psoriasis to improve with discontinuation of the TNF inhibitor (as was noted in the majority of patients); rather, discontinuation would have been expected to result in worsening of psoriasis.

