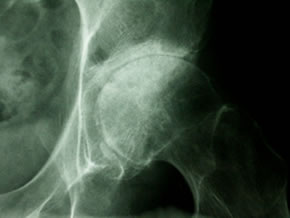
Large scale, independent studies of glucosamine and/or chondroitin have not shown a definitive benefit for the treatment of painful knee osteoarthritis (OA) and the effect of retarding knee OA progression remains controversial. Despite this, the use of glucosamine as a complementary/alternative medicine is widespread, amounting to a multi-million dollar industry. Many users take glucosamine for OA at sites other than the knee, sites which have received little to no study of efficacy. Here, Rozendaal et al (Ann Intern Med 2008; 148: 268) report the findings of a randomized clinical trial examining the effect of glucosamine sulfate on hip OA symptoms and radiographic progression.
Methods
Patients without end-stage hip OA were randomized on a 1:1 basis to receive glucosamine sulfate (750 mg twice a day; manufacturer Nutricia) or identical placebo in a double blind fashion for 2 years. Outcomes included pain and function measured using the Western Ontario and McMaster (WOMAC) Osteoarthritis Index subscales, 24-month progression of joint space narrowing in the most symptomatic hip, and use of pain medications. Minimally clinically important changes were set at 10 point differences in WOMAC scales and a change in joint space narrowing of 2.5 mm over 24 months.
Results
222 patients were randomized equally to each group, of whom 207 (93%) completed the trial. Drop-outs were equal between groups. Adherence to therapy was high (>80%). Women comprised 69% of subjects with a mean age of 63 years. The majority of patients reported disease of > 3 years duration. Baseline minimum joint space narrowing and WOMAC scores were balanced between groups. Approximately half of patients had mild radiographic OA (Kellgren-Lawrence grade of 1). Twenty patients underwent total hip replacement during the course of the trial (7 in the placebo group and 13 in the active treatment group).
There were no statistical or clinically important differences between glucosamine and placebo in any of the primary outcomes (WOMAC pain, function, or radiographic progression) over the 24 months of the trial. Neither were there statistical differences in secondary outcomes (stiffness, pain (VAS)). These differences did not change when corrected for adherence or for other potential confounders. There were no significant differences in the occurrence of adverse events between the two groups.
Conclusions
Glucosamine sulfate was not efficacious in treating the symptoms or retarding radiographic progression of hip OA over two years of use.
Editorial Comment
Large, randomized trials of glucosamine that lack pharmaceutical sponsorship have largely shown no effect of glucosamine for analgesia or structural modification in knee OA. One of the criticisms of the landmark GAIT trial in knee OA was that glucosamine HCL was used instead of glucosamine sulfate. Yet here, this difference appears to be irrelevant. One criticism of the trial presented here is that a large number of patients with mild radiographic disease were included. However, all patients were symptomatic, with baseline WOMAC pain and function scores consistent with other trials, and since the objective was to investigate radiographic progression, one would still expect patients with even mild radiographic OA to demonstrate differences in progression rates if there was a beneficial effect of the drug.
Should hip OA patients who have derived subjective benefit from glucosamine stop the drug based on these results? Probably not, although frequent reappraisal of whether its use is helpful is advised. There appears to be little downside regarding toxicity for continuing the drug. However, taking a drug with little or no effect for a prolonged period of time may have a detrimental effect on the pocketbook.

