- Joint Pain is Strongly Associated with Body Weight
- Obesity Is a Risk Factor for Osteoarthritis
- The Benefits of Weight Loss
- Would My OA Patient Benefit from Losing Weight?
- Calculate your Body Mass Index (BMI)
- How Can I Help My Patients to Manage Their Weight More Effectively?
- What About Weight Loss Medications?
- What if My Patient Is Not Willing to Lose Weight?
- For More Information About Safe and Effective Methods of Weight Loss
- References
Joint Pain is Strongly Associated with Body Weight
Being only 10 pounds overweight increases the force on the knee by 30-60 pounds with each step.
Osteoarthritis is the most common joint disorder with symptoms in the hands, knees, hips, back, and neck. It is unclear exactly how excess weight influences OA. Clearly, being overweight increases the load placed on the joints such as the knee, which increases stress and could possibly hasten the breakdown of cartilage.(ref. 1) For example, it is estimated that a force of nearly three to six times one’s body weight is exerted across the knee while walking; an increase in body weight increases the force by this amount.(ref. 2) However, overweight has also been associated with higher rates of hand OA in some studies (refs. 3 and 4) suggesting the involvement of a circulating systemic factor as well.(ref. 5)
Obesity Is a Risk Factor for Osteoarthritis
Overweight women have nearly 4 times the risk of knee OA; for overweight men the risk is 5 times greater.
Being overweight is a clear risk factor for developing OA. Population-based studies have consistently shown a link between overweight or obesity and knee OA. Estimating prevalence across populations is difficult since definitions for obesity and knee OA vary among investigators. Data from the first National Health and Nutrition Examination Survey (HANES I) indicated that obese women had nearly 4 times the risk of knee OA as compared with non-obese women; for obese men, the risk was nearly 5 times greater. (ref. 6) In a study from Framingham MA, overweight individuals in their thirties who did not have knee OA were at greater risk of later developing the disease. (ref. 7) Other investigations, which performed repeated x-rays over time also, have found that being overweight significantly increases the risk of developing knee OA. (refs. 8 and 9) It is estimated that persons in the highest quintile of body weight have up to 10 times the risk of knee OA than those in the lowest quintile. (ref. 5)
The Benefits of Weight Loss
Even small amounts of weight loss reduce the risk of developing knee OA. Preliminary studies suggest weight loss decreases pain substantially in those with knee OA.
If obesity increases the development and progression of knee OA, can weight loss reverse these effects? In the Framingham study, Felson and colleagues noted that among women with a baseline body mass index (BMI) greater than or equal to 25, weight loss was associated with a significantly lower risk of knee OA. (ref. 10) For a woman of normal height, for every 11 lb weight loss (approximately 2 BMI units), the risk of knee OA dropped > 50%. Conversely, a comparable weight gain was associated with an increased risk of later developing knee OA (odds ratio 1.28 for a 2 BMI weight gain). The investigators concluded that in elderly persons, if obese men (i.e., BMI greater than 30) lost enough weight to fall into the overweight category (BMI 26-29.9) and men in the overweight category lost enough weight to move into the normal weight category (BMI less than 26), knee OA would decrease by 21.5%. Similar changes in weight category by women would result in a 33% decrease in knee OA. A handful of studies have indicated that weight loss substantially reduced reports of pain as well. Thus, weight loss potentially offers an important modifiable factor in the behavioral treatment of knee OA.
Would My OA Patient Benefit from Losing Weight?
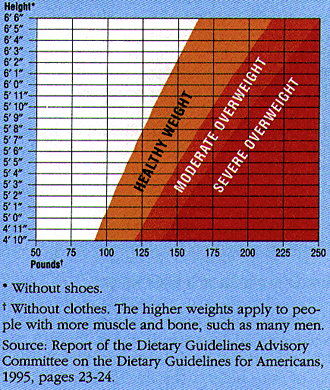
Weight/Height Tables. Determining whether a patient would benefit from weight loss involves making some informed decisions. One method that offers general guidelines is to determine whether a patient’s weight falls into the “healthy weight ranges” currently recommended for adults. These ranges, which were revised and updated in 1995, are presented in the Optimal Weight/Height Table below. In general, within each range the lower weights are for women, while the higher weights are for men.
Federal Guidelines on Obesity The first Federal Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults were released in March, 1998 by the National Heart, Lung, and Blood Institute (NHLBI), in cooperation with the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (ref. 11) These guidelines proposed that health care providers use three measures to assess overweight: (1) body mass index (BMI); (2) waist circumference, and (3) patient’s risk factors for diseases and conditions associated with obesity.
- Body Mass Index (BMI) – The use of BMI as an indicator of overweight is based on extensive research linking BMI with associated health risks. BMI is calculated by dividing the patient’s weight in kilograms is divided by height in meters, squared. Tocalculate your patient’s body mass index, insert your patient’s weight in pounds and height in feet and inches.According to the new guidelines, overweight is a BMI of 25-29.9 while obesity is a BMI of 30 or greater. (A BMI of 30 is about 30 lbs overweight). It is recommended that BMI be calculated in all adults to assess overweight and those who are normal weight should be reassessed every 2 years.
- Waist Circumference – Waist circumference is another measure which provides important information about the associated health risks. Waist circumferences is closely linked with abdominal fat (i.e., having an “apple” shape), which is an independent predictor of disease risk. A waist circumference of greater than 40 inches (102 cm) in men and greater than 35 (88 cm) in women signifies increased risk in those who have a BMI of 25 to 34.9.
- Risk For Obesity-Related Diseases – Additional markers of health risk also need to be taken into consideration when assessing the appropriateness of your patient’s weight. Be certain to evaluate risk factors such as elevations in blood pressure or blood cholesterol, or family history of obesity-related disease. At a given level of overweight or obesity, patients with additional risk factors are considered to be at higher risk for health problems, and would benefit from weight loss as well as modification of risk factors.
How Can I Help My Patients to Manage Their Weight More Effectively?
- Assess weight and advise all overweight and obese persons to lose weight
- Review health benefits emphasizing the link between weight loss, exercise and improvement in joint pain
- Suggest an initial weight loss goal of 10% and a safe rate of weight loss
- Review changes in eating, behavior, and physical activity that are necessary to lose weight
- Discuss how to proceed (e.g., on own or in a program) and maximize support
- Monitor progress with follow-up visits
There are many things you can do to facilitate safe and effective weight management practices with your patients with arthritis. First, address weight directly as an important component of arthritis management. Clearly advise all overweight and obese patients to lose weight. Second, review the health benefits of small weight losses with patients, emphasizing the positive effects of reduced weight and exercise on OA-symptoms such as pain. Third, suggest an initial weight loss goal of 10%; if patients are successful achieving this, further weight loss can be attempted, if appropriate. A recommended rate of weight loss is 1-2 lbs per week. (ref. 12) Fourth, discuss with patients how they can best achieve weight loss. Successful strategies for weight loss include calorie reduction, increased physical activity, and behavior therapy designed to improve eating and physical activity habits. (ref. 11) Specifically, you should suggest that overweight and obese patients:
- Participate in moderate physical activity, progressing to 30 minutes or more on most or preferably all days of the week.
- Cut back on both dietary fat and total calories. While reducing dietary fat can help reduce calories and is heart-healthy, this method alone – without reducing calories – will not produce weight loss.
- Make weight-maintenance a priority after the first 6 months of weight-loss therapy.
It may be helpful to discuss whether a structured weight management program in your community that offers education and support would be helpful. They are many inexpensive options available in most communities (i.e., commercial or hospital-based programs). In larger centers, clinical weight management services may be available. Clinical programs offer comprehensive assessment and treatment approaches by a multi disciplinary team. Additional options such as the use of very-low-calorie diets, gastric surgery, or pharmacotherapy are often available. These programs are especially appropriate for individuals with co-morbid health conditions or those who are severely overweight. While services are often more costly in clinical programs, in some cases they may be covered by health insurance.
What About Weight Loss Medications?
The clinical guidelines suggest that all patients try lifestyle-based approaches for at least 6 months before embarking on drug therapy. Weight loss drugs approved by the FDA for long-term use may be tried as part of a comprehensive weight loss program that includes dietary therapy and physical activity in carefully selected patients (BMI >30 without additional risk factors, BMI >27 with two or more risk factors) who have been unable to lose weight or maintain weight loss with conventional non-drug therapies. In general, if a patient does not lose 4.4 lbs (2 kg) in the first four weeks of treatment, the patient can be considered a non-responder to pharmacotherapy. Drug therapy may also be used during the weight maintenance phase of treatment. Safety and effectiveness beyond one year of total treatment have not been established. (Frequently, weight loss drugs are not covered by health insurance.)
What if My Patient Is Not Willing to Lose Weight?
Because lifestyle changes are ultimately required for successful weight maintenance, your patient’s readiness to make these changes and willingness to commit to them over the long-term are crucial. Studies have shown that health promotion messages are most effective when specifically targeted to the patient’s level of readiness. For patients who are not ready to lose weight at this time, the goal should focus on strategies to avoid further weight gain through healthy eating and more physical activity. Because level of readiness changes over time, it is important to reassess motivation periodically. While you are respectfully accepting of your patient’s decision to not lose weight at this time, be sure and reinforce that when they are ready to lose weight, you will be there to support and help them achieve their goals.
For More Information About Safe and Effective Methods of Weight Loss
Methods for Voluntary Weight Loss and Control (National Institutes of Health Technology Assessment Conference.)
Institute of Medicine. Weighing the Options: Criteria for Evaluating Weight-Management Programs. Washington,D.C., National Academy Press; 1995.
References
- Creamer P, Hochberg MC: Osteoarthritis. Lancet 1997;350:503-508.
- Felson DT: Weight and osteoarthritis. J.Rheumatol. 1995;43:7-9.
- Carman WJ, Sowers M, Hawthorne VM, Weissfeld LA: Obesity as a risk factor for osteoarthritis of the hand and wrist: a prospective study. Am.J.Epidemiol. 1994;139:119-129.
- Cicuttini FM, Baker JR, Spector TD: The association of obesity with osteoarthritis of the hand and knee in women: a twin study. J.Rheumatol. 1996;23:1221-1226.
- Felson DT: Weight and osteoarthritis. J.Rheumatol. 1995;43:7-9.
- Anderson J, Felson DT: Factors associated with osteoarthritis of the knee in the First National Health and Nutrition Examination (HANES I). Am.J.Epidemiol. 1988;128:179-189.
- Felson DT, Anderson JJ, Naimark A, Walker AM, Meenan RF: Obesity and knee osteoarthritis: The Framingham study. Ann.Int.Med. 1988;109:18-24.
- Felson DT, Chaisson CE: Understanding the relationship between body weight and osteoarthritis. Baillieres Clinical Rheumatology 1997;11:671-681.
- Schouten JS, van den Ouweland FA, Valkenburg HA: A 12 year follow up study in the general population on prognostic factors of cartilage loss in osteoarthritis of the knee. Ann.Rheum.Dis. 1992;51:932-937.
- Felson DT, Zhang Y, Hannan MT, et al: Risk factors for incident radiographic knee osteoarthritis in the elderly: the Framingham Study. Arthritis Rheum. 1997;40:728-733.
- National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Disease: Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report, Bethesda, MD, U.S. Department of Health and Human Services; 1998.
- Institute of Medicine: Weighing the Options: Criteria for Evaluating Weight Management Programs, Washington, D.C., National Academy Press; 1995.

